What is the
true cost of
Bronchoscopy?
A new study conducted at Guy’s and St Thomas’ NHS Foundation Trust Department of Anaesthesia has found that single-use flexible bronchoscopes are more cost-effective and associated with a lower risk of infection than reusable flexible bronchoscopes.
Download study summary
See the full report of the study findings published in the Anaesthesia journal.
Cost-effectiveness of Reusable vs. Single-Use Bronchoscopes
Gabriel Brown, Senior Health Economist at Ambu, discusses the findings of a systematic review and cost-effectiveness analysis of reusable vs. single-use flexible bronchoscopes.
Video insights
Watch recordings from a live event where the study’s authors presented some background for their research and were joined by Cori Ofstead, an expert in the field of cross-contamination.
Perspective
Cori L Ofstead (MSPH) presents research findings on the effectiveness of reprocessing bronchoscopes.
38 minutes
Insight
Two of the study authors, Dr Imran Ahmad and Dr Kariem El-Boghdadly, tell the story of how they factored in the risk and cost of infection to their analysis.
20 minutes
Conclusions
Professor of health economics, Lars Ehlers, presents the conclusions on the cost effectiveness calculations presented in the study
7 minutes
Results of the study
• Capital cost comparison
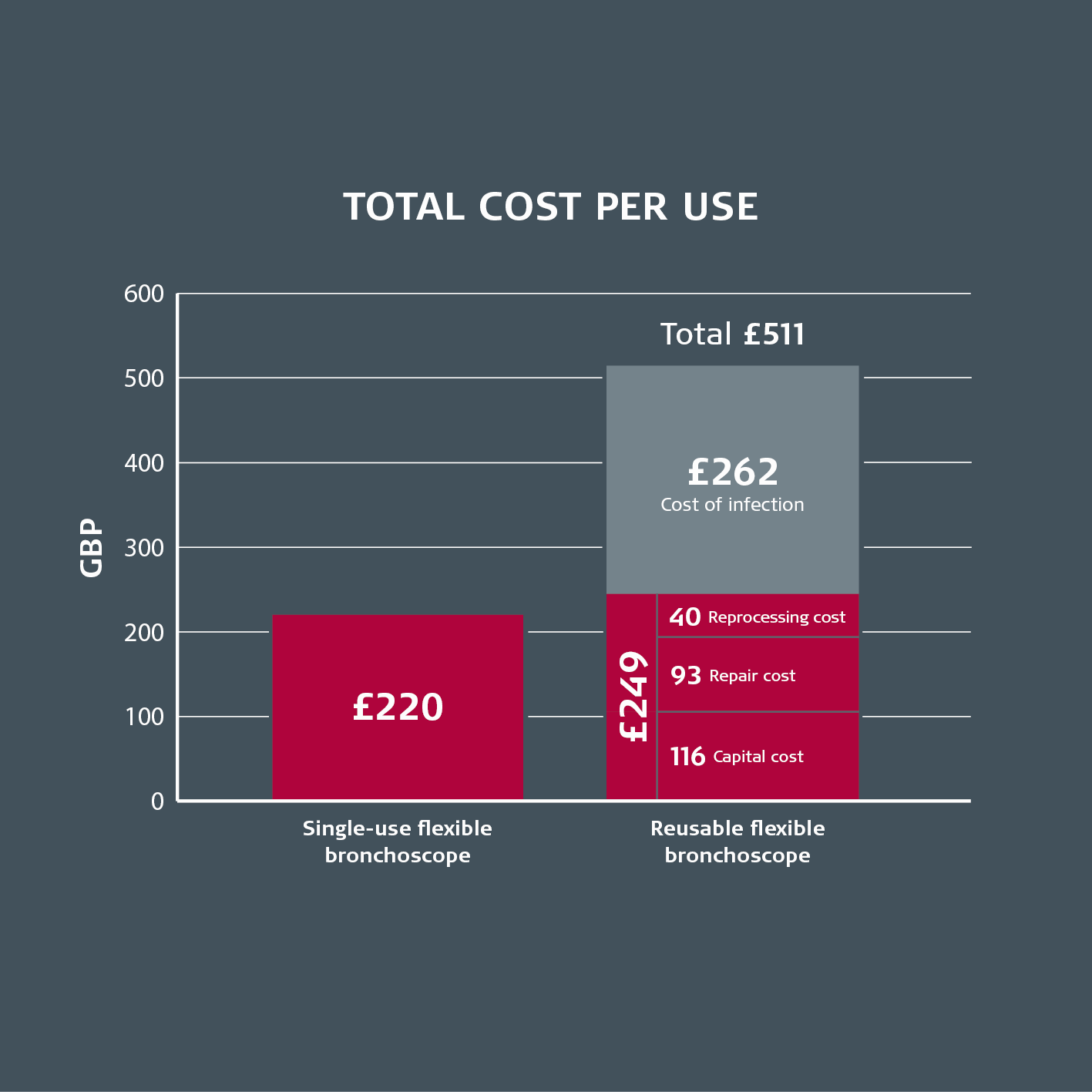
The study found that when capital costs alone are considered, the cost per patient with a reusable flexible bronchoscope is £249 compared to £220 with an Ambu® aScope™ 4 single-use bronchoscope1.
• The cost of cross contamination
When the cost of treatment of infection (£262) is taken into account, the total cost per patient with a reusable flexible bronchoscope rises from £249 to £511. That is a total cost savings of £291 per procedure.
• Conclusion
The study concluded that single-use bronchoscopes offer a number of advantages over reusable ones: “The findings from the study suggests benefits of single-use FBs in terms of cost-effectiveness, cross-contamination and resource utilisation.”
1The cost per use of a single-use flexible aScope™ single-use bronchoscope used in the study was provided by Ambu®.
Why was this study conducted?
The true cost of bronchoscopy can be difficult to determine
Routine bronchoscopies are generally regarded as safe and cost-efficient procedures that help patients and even save lives. However, determining the true cost of procedures performed with reusable flexible bronchoscopes can be challenging because they:
• Are often split across departments, budgets, tied into large procurement contracts
• Include variable costs associated with reprocessing, such as cleaning consumables, work time and repairs.
• Do not include the cost of infection, which can arise as a result of cross-contamination
Getting to the root
of the problem
The new study conducted at Guy’s and St Thomas’ NHS Foundation Trust Department of Anaesthesia offers some clarity.
The study is the first to combine a systematic review of relevant literature with a quantifiable micro-costing analysis in order to calculate the risks and costs linked to cross-contamination and infection.
Download a summary of the study
See the full report of the study findings published in the Anaesthesia journal.





